When she was in college, Tania Betancourt’s grandfather was admitted to the hospital for brain cancer treatment. Seeing him lose control of his body and himself—because “your brain is you”—was awful, she says. She wanted to see cancer treatment that could target his illness more directly.
“Our current options to treat cancer are not great. Chemotherapeutic agents are inherently toxic agents that we’re injecting into our body to try to kill cancer, and we know from the beginning that they will affect our wellbeing,” says Betancourt, Ph.D., a biomedical engineer who leads research at the Texas State University Biomaterials and Nanomedicine Laboratory. Dr. Betancourt guides both undergraduate and graduate students in research, as well as in designing tiny carriers called nanomaterials that go into the body with the aim to detect, monitor, and destroy cancer cells without harming healthy tissue.
Dr. Betancourt is one of a group of Texas State University professors and other Texas researchers leading work in targeted cancer treatment research. Engineers, chemists, and other biomedical investigators from institutions extending from Houston’s Texas Medical Center to Central Texas are focused on preventing and treating cancer at its source. They probe strategies to make nanoparticles interact more effectively with the body, sharing real-world techniques that help students build a biomedical future.
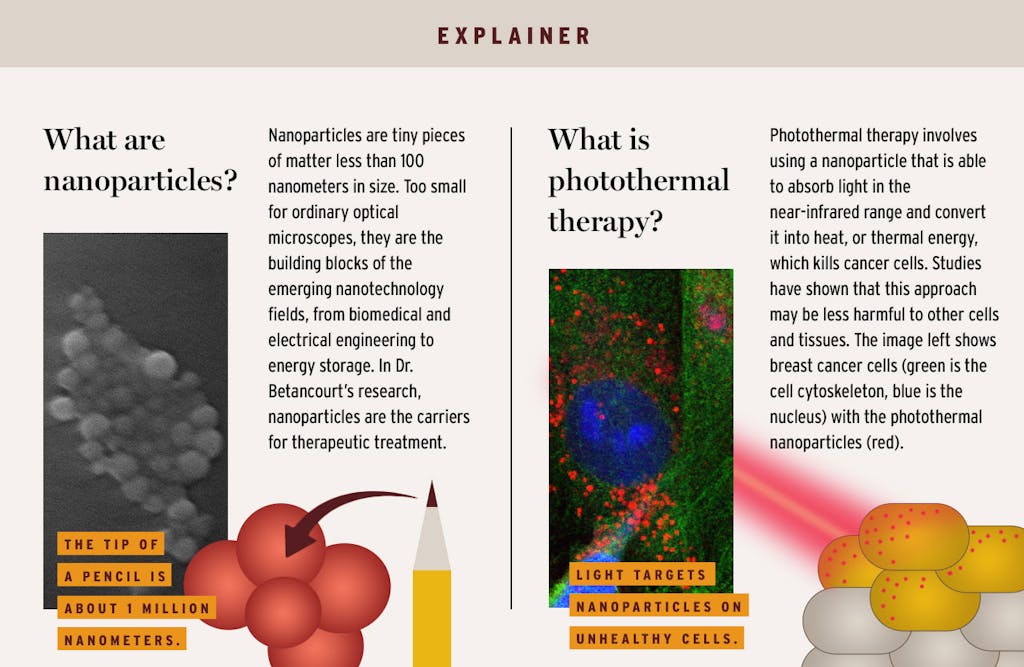
When Dr. Betancourt was herself in graduate school twelve years ago, researchers believed nanomedicines could be injected into a patient’s blood vessels, travel the circulatory system, and land at the site of a target tumor. Known as enhanced permeability and retention effect (EPR), this theory performed better in research on mice than humans.
But things change rapidly in biomedicine. Now Dr. Betancourt is collaborating with researchers at Texas State University and the University of Texas at Austin on photothermal therapy, which uses lasers to induce heat generation within tiny carriers at the site of various medical conditions, including cancer. As they work to better direct nano materials and light into human systems, researchers build their way toward more effective immunotherapy, or training the body’s immune system to target tumors or other conditions. While the first immunotherapy for cancer was approved in 2011, it doesn’t yet work for all patients.
“I wanted to utilize concepts of physics, chemistry, biology, and engineering, and apply them to problems—like cancer—that are relevant to all of us.”
Despite setbacks, Dr. Betancourt thrives on the investigative work. “There are many things we still don’t understand. But scientifically, working with the human body is exciting—it’s a complicated system we’re trying to interact with,” she says. “It’s thrilling when we can make an impact.”
Since she was a freshman at Texas A&M, Dr. Betancourt has wanted to do the world-helping work of an engineer. After a youth spent in Colombia, she arrived in Texas with an interest in chemistry and chemical processes. Studying chemical engineering, she landed a job after graduation at a manufacturer of insecticides and herbicides. But something was missing, and she quickly realized she needed to feel passionately toward her research.
“I wanted to utilize concepts of physics, chemistry, biology, and engineering, and apply them to problems—like cancer—that are relevant to all of us,” she says.
Returning to school, Dr. Betancourt focused on biomedical engineering and earned master’s and doctorate degrees at the University of Texas at Austin. She emerged with a strong awareness of how to work with the biological species—and how molecules interact—to treat tumors or detect diseases.
Today, collaborating with James Tunnell, Ph.D., an associate professor and Roberta Woods Ray Centennial Fellow in Engineering at the University of Texas at Austin, Dr. Betancourt designs and makes nanoparticles for work using lasers to treat cancer.
In two articles published in November 2020 (article one and article two), the team found that their technique caused cancer cell death in such a way that it could potentially stimulate an immune response. Among other results, that immune reaction reduced internal adenosine trisphosphate (ATP), a material cancer cells need to thrive. That positive reaction was due in part to Dr. Betancourt’s very precise skill set—allowing her to design and make nanomaterials that can be directed to a tumor, locally induce cell death, and stimulate molecular pathways that can engage the immune system to attack cancer.
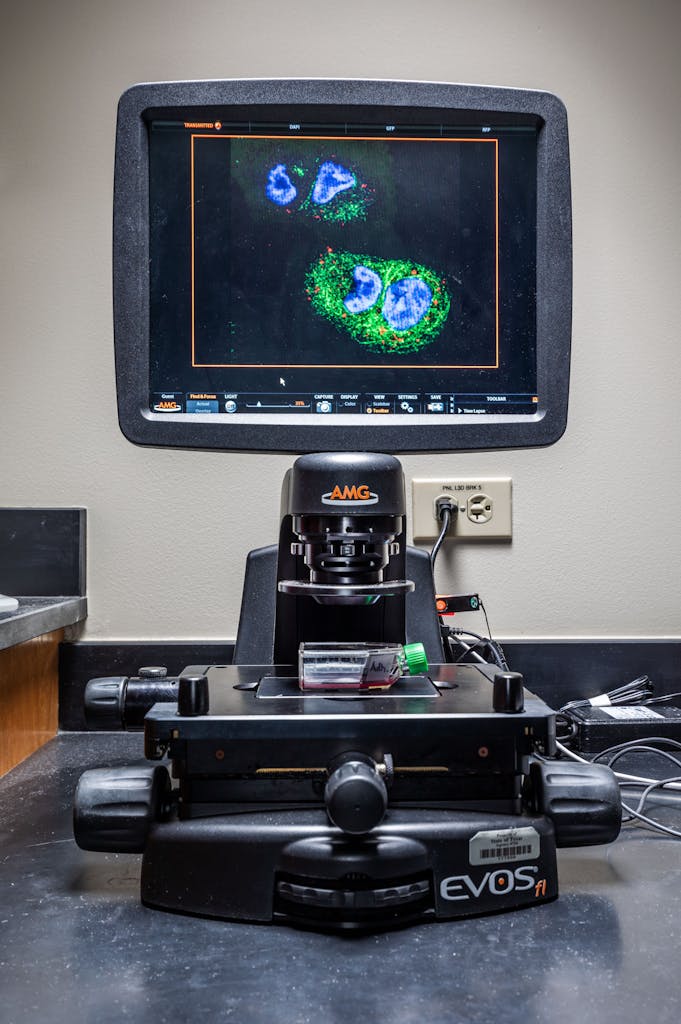
“Treatments that target the immune system (called immunotherapies) have become a primary treatment option showing long term survival benefits; however, most people do not respond,” says Dr. Tunnell. “Dr. Betancourt’s work shows promise in stimulating the immune system in a way that could increase the response rates of these already FDA-approved immunotherapies.”
Organic chemist Jennifer Irvin, Ph.D., also participated in the November publication, having helped to prepare nanomaterials designed by Dr. Betancourt. An associate professor and director of the Texas State Materials Science, Engineering, and Commercialization Program, Dr. Irvin frequently works with Dr. Betancourt on research in disease treatment and detection of disease markers. “If we can come up with a screening test for healthy people, we can catch conditions earlier and start treatment sooner,” Dr. Irvin says.
Currently, Irvin and Betancourt are collaborating to develop a polymer-made analytic device to detect markers of disease, such as certain proteins overexpressed by cancer cells. Such biosensors would enable real-time, point-of-care testing at a low cost, as Betancourt and Irvin wrote in a 2019 publication, “In theory, detected biomarkers could be for cancer or any disease we are interested in focusing on,” explains Dr. Betancourt.
With results that could take many years, maybe decades to reach a market, Dr. Betancourt admits the work is a process. “But if these technologies are further developed and commercialized, they could be used for detection and treatment,” she explains. “I think eventually, we can use thermotechnologies for almost any type of cancer.”

Working with Texas State University students—even ambitious first year students—is extremely important to Betancourt, who provides direction to students as they conduct research. She helps them analyze data and troubleshoot problems, identifies alternative pathways, and teaches methods for presenting technical information. “I provide hands-on training to help students become competent scientists or engineers who can contribute in their own right,” she says. “I love mentoring students—many of them may not have had any experience with science, and it is so rewarding to watch them learn and grow, realizing that they can have a career in this field.”
Many of these students will take the skills honed working with Dr. Betancourt to jobs in biomedical research, notes Dr. Irvin. “Much of our research doesn’t necessarily make it to therapeutic treatments, but the tools and techniques students learn are universal: problem-solving and making and assessing materials. They’ll be able to get a job at a pharmaceutical or biotech company and work using those same skills.”

“When our students realize what they can accomplish with their knowledge and skills, they can make a difference in the world.”
Master’s student Emilio Lara is a good example. Following community college work, he arrived at Texas State in 2018 as an undergraduate and asked to join Dr. Betancourt’s research; by fall 2020, he was a co-author on three publications and applying to Ph.D. programs. Two of the papers are about creating immune system response to kill cancer cells, another addresses large-scale fabrication of nanomaterials.
“I’ve done a lot since I first got to Texas State up to today—I can attribute that to my hard work, but also to Dr. Betancourt and her lab,” he says. “From where I was when I started at the university, not knowing how to get there, she’s been the best at getting me there.”
While Dr. Betancourt says she may not reach the market for some time with her work, beneficiaries of her ongoing research include Texas State scholars: “When our students realize what they can accomplish with their knowledge and skills, they can make a difference in the world.”








