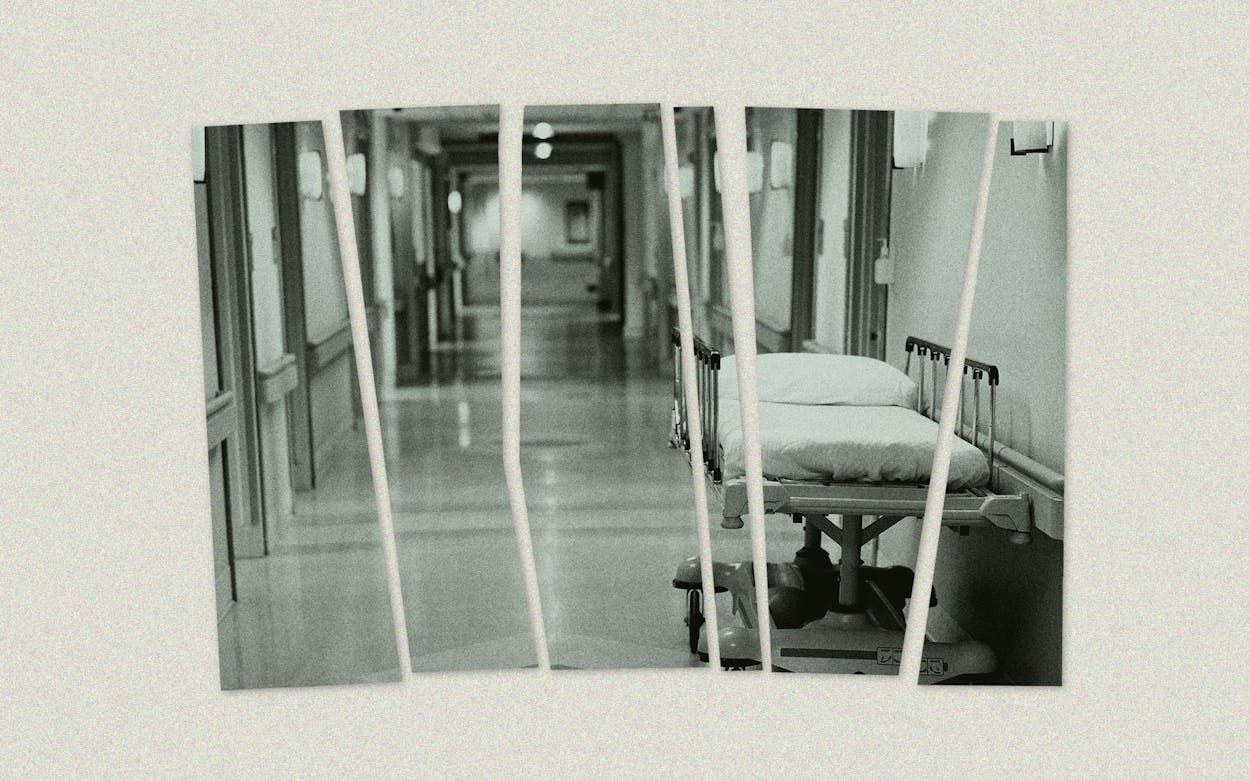
Ted Matthews couldn’t have imagined a few months ago that today he’d be using an empty patient room at Anson General Hospital as his bedroom. He and his wife were enjoying a quiet retirement in Waco when he got a call last summer about the hospital’s grim prognosis. Its CEO was taking a position elsewhere as it faced rising operating costs and declining patient numbers. It might soon be forced to close.
In the nineties and early aughts, Matthews and his wife had raised their son in Anson, home to 2,300 residents about 25 miles north of Abilene. He’d worked then as an administrator at Anson General, and even after he’d moved on to running Eastland Memorial, eighty miles to the east, he continued to feel connected to the community. So when the hospital board asked him whether he’d consider returning as interim CEO, Matthews agreed. “How do you say ‘no’ to your hometown?” he asks with a chuckle.
With his wife staying behind in Waco, and not knowing exactly how long his transitional tenure would last, Matthews moved into the low-slung beige-brick hospital building and got to work. Though it can theoretically accommodate 20 to 25 beds, Anson General often admits only a single patient each day, if that. With 65 full-time employees, that low patient volume means making payroll each month can be a struggle. But Matthews says his staff knows how to stretch a dollar, and everyone pitches in. He’ll occasionally sweep floors in the ER and hand out food trays to patients, while nurses will help him with spreadsheets. “It is just whatever we need to do to keep our facility going,” Matthews says.
Anson isn’t unique in facing such challenges. Rural hospitals across the country—particularly in Texas—are in crisis. A recent study from the Chartis Group, a Chicago-based health care consulting firm, determined that more than 50 percent of Texas’s rural hospitals are vulnerable to closure. Since 2010, 26 have shuttered, according to the Texas Organization of Rural and Community Hospitals, known as TORCH. That’s more than in any other state in the country, which has seen nearly 150 hospitals close their doors for good over the same period. Were it not for a newly launched federal program, the Anson hospital and others like it might soon be added to these numbers. “It is a really, really good option for us,” Matthews says. “In our case, it was the only option.”
Congress established a Rural Emergency Hospital designation in 2021 in an attempt to stem the tide of closures. Starting in January of this year, hospitals with fewer than fifty beds that aren’t located within a metropolitan area, or those that had already been designated Critical Access Hospitals (a federal designation established in 1997), are eligible for an additional 5 percent for each outpatient service provided to Medicare patients—who typically constitute a significant percentage of those visiting rural hospitals—as well as a flat monthly payment, about $273,000.
John Henderson, president of TORCH, says this program could serve as a “safety valve” for several hospitals in the state, but notes that it comes with a significant trade-off. Participating hospitals must cease providing inpatient services in favor of a financially leaner emergency-room-focused model of care. Many of the hospitals now at risk spend a lot of money maintaining underused facilities, and cutting those costs in tandem with the federal support could prove a sustainable path to staying in business. While there will still be hospital beds in REH facilities, the average patient’s stay can’t exceed 24 hours. Anyone needing long-term care must be quickly transferred to an available inpatient facility, which in some cases could be hours away.
According to TORCH, of the 158 rural hospitals in the state, four—Anson General, Crosbyton Clinic Hospital, Falls Community Hospital in Marlin, and St. Mark’s Medical Center in La Grange—have decided to convert into REH facilities. Henderson suspects that a dozen Texas hospitals may make the change during the next couple of years, though usually as a last resort.
For decades, rural hospitals have had to contend with the strains of increased operating costs—many of those associated with keeping up with technological advances in health care—at the same time that their communities have seen population levels stagnate or decline. These hospitals also struggle to compete with the state’s metropolitan areas in attracting doctors, nurses, and other medical staff, which drives up labor costs. And while the big cities and their suburbs can support a host of specialized hospitals and clinics, “in a rural community, you have one hospital that has to care for the entire community,” says Kia Parsi, a physician and executive director of the Texas A&M Rural and Community Health Institute. “As a society, we have to decide: How do you fund that? Because the current structures that we have in place are not really adequate.”
COVID-19 outbreaks kept some rural Texas hospitals afloat—none have closed in the last three years—thanks to federal stimulus money and the relatively high number of patients that these usually low-volume facilities were caring for. “They all came out of the pandemic, but we’re seeing, especially in 2022 and 2023, a return to that severe risk of closure status for a half dozen or so,” Henderson says.
Jones County once had three hospitals, but Anson General is the only one remaining. Even with much larger Abilene nearby, the hospital can save lives that would be in greater danger if the patients had to travel farther for care. In recent weeks, three patients have been airlifted out of the hospital, and in each case they were successfully stabilized, but “it could have been very different if we had not had our emergency room here,” Matthews says. Under the new REH designation, which Anson General received this week from the Centers for Medicare & Medicaid Services, they’ll be able to maintain their emergency room, as well as its attached outpatient health clinic.
Matthews regrets losing the ability to admit patients, and he laments that the hospital will no longer be able to offer “swing beds,” an arrangement that allows patients—often elderly—who are recovering but who still need skilled care to remain in the hospital. But the cost of maintaining those services was unsustainable. “From a financial standpoint, it was very, very challenging,” Matthews explains. He says they’ve already had to let eight employees go, and that number will certainly grow in the coming months, even with the federal assistance.
Another Texas hospital that faces an even more imminent closure without the REH program is St. Mark’s Medical Center in La Grange, about halfway between Austin and Houston. “We just don’t have the balance sheet that we need to be able to wade through these troubling waters,” says Mark Kimball, the hospital’s CEO. The 38-bed nonprofit hospital, built in 2005, isn’t part of a major health care system, nor is it funded by a local tax district, a critical source of money for many community hospitals. It likely would have had to close its doors during the first quarter of 2023, but if it’s approved as a Rural Emergency Hospital, the federal financial support should keep the lights on.
Still, the hospital has already eliminated 64 jobs in shuttering its inpatient services, as well as all orthopedic and surgical services. Kimball says the hospital board jumped at the opportunity to enroll as an REH. In enabling St. Mark’s to continue to provide emergency and outpatient care as the only hospital serving Lee and Fayette counties, it would preserve the jobs of the 80 remaining hospital employees. If St. Mark’s closes, patients would need to drive another twenty miles to Smithville for care.
For facilities that can get by financially without converting, the REH designation usually doesn’t make sense. Golden Plains Community Hospital in Borger—a Panhandle town of approximately 12,500 about an hour northeast of Amarillo—faces some of the same financial strains as other rural hospitals but isn’t seeking an REH designation. “We have opted not to go there quite yet,” says Don Bates, the hospital’s CEO. “Honestly, I hope we don’t have to because I like being able to offer a full complement of inpatient and outpatient services.”
The A&M Rural and Community Health Institute, along with colleagues at Texas Tech, is organizing webinars for hospitals such as Golden Plains that might have questions about the new designation. While the program could be a much-needed lifeline, Parsi worries that local ambulance services will be tied up transporting patients from REH facilities to larger hospitals. In some instances, this will require hours-long drives to distant inpatient hospitals. For Jones County, which has three ambulances operating in distinct zones, the increased transports could mean prolonged response times during emergencies.
Parsi also notes that, as we saw during the COVID-19 pandemic, rural hospitals with inpatient services are desperately needed when hospital beds are in short supply nationwide. REHs won’t be able to provide those beds. Still, Parsi says that after the Critical Access Hospital designation was established in 1997, the program evolved to meet unanticipated needs and allowed rural facilities to provide more care. For instance, subsequent legislation granted these hospitals flexibility regarding the length of a patient’s stay and how swing beds could be used. “I am hopeful that in the future this REH designation will add some of the services that Critical Access Hospitals [that convert] are losing,” he says.
As Parsi is quick to point out, the expansion of Medicaid eligibility in Texas could go a long way toward easing the financial strain on rural hospitals. But even though polls show that the vast majority of Texans support such expansion—which projections show could insure more than 1 million uninsured Texans and bring more than $5 billion of federal money into the state’s health care system—leading Republican state lawmakers have repeatedly refused to enact it. Each of the eight states with the highest rates of rural hospital closures since 2010 has declined to expand its Medicaid program, according to the Chartis Group study.
Texas has the largest rural population in the country, so the rural health crisis hits the state especially hard. In addition to poor health outcomes, both Kimball and Matthews highlighted the economic devastation that can follow a hospital closure. Those in the rural health care industry often say that small towns stand on the “three-legged stool” of health care, education, and industry. If you take one of those legs away, the whole community could falter. The REH program will help keep that stool upright in some of these communities, but without bigger systemic remedies, experts agree that the underlying crisis will persist.
- More About:
- Politics & Policy
- Health
- Medicine
- La Grange
- Abilene