When Tricia Gschwind pulled up to a Whataburger along I-35 in Round Rock one morning last May, she wasn’t craving a breakfast platter. She was there to make an exchange. “I never bought drugs at a Whataburger,” she said, easing into a parking space. “I assume this is what that’s like.”
Gschwind (pronounced GISH-wind) stepped out of her car, straightening her royal blue cat-eye sunglasses as strands of her hair flitted in the breeze. She recognized a Toyota SUV that arrived some thirty seconds later. A graying beekeeper in a polo shirt approached. His name was Jim Colbert, and after a quick hello, they got right down to business. Into Gschwind’s hands he delicately placed two four-inch-long wooden palettes—imagine tiny, mesh-covered mancala boards—each holding about fifty live honeybees, buzzing softly.“I guess this is drone season,” Gschwind said, alluding to the previous batch of bees she’d purchased from him, which had included some stinger-less males. Gschwind needed bees that could sting. “Is that why it’s not unusual for me to find so many drones in the mix?”
“There probably won’t be many in here,” Colbert responded. “I took them all out of a different hive last time.” Gschwind nodded that she understood, and, since she’d already paid him $45 through an online payment app, their transaction concluded in less than a minute. “Just call me with what you need,” he said, waving goodbye.
Gschwind turned back to her car, where she arranged the palettes in a cupholder, like two thick, vibrating chopsticks. She considered the bees to be medicine, as necessary to her well-being as insulin is for a diabetic. She understood that this opinion could make her seem crazy. The protocol she’d been using for the past eight months was ten stings along the spine, three days a week. After about three years of this regimen, she believed, she would be healed from Lyme disease, a condition that had been making her life a living hell for the past decade.
Two days earlier, I’d visited 36-year-old Gschwind in her tidy one-bedroom Austin apartment. Books about debilitating illnesses lined her shelves, and on her kitchen counter sat a wood-and-wire-mesh cage the size of a shoebox, full of bees. With her was a friend, Marla Avery, who had stripped down to a sports bra and was numbing her lower back with an ice pack. An EpiPen was placed within reach, in case a sting sent one of them into anaphylactic shock. While Avery leaned over the counter, psyching herself up with deep breaths, Gschwind reached a pair of self-closing tweezers into the small cage and pulled out a buzzing candidate.
“We’re repositioning them so that their stingers are in the right spot,” Gschwind said. She fumbled with the insect, wincing and whisper-singing “oh honey” and “sweetheart” as it wriggled around, then continued her businesslike explanation. “We try to make it so that the tweezers hold them between their head and their thorax,” she said.
Avery was 41 and had been diagnosed with Lyme in 2013, though her symptoms dated back years before that. She told me that it had taken a few months to work up to ten stings; she thought the bee venom was setting off something called a Jarisch-Herxheimer reaction, a response to antimicrobials like antibiotics, in which the bacteria being destroyed release their contents into the bloodstream and cause flu-like symptoms. (It’s not scientifically documented whether venom in fact triggers the same reaction.) “I’m starting to handle it better than at first,” Avery said. “Like I’m not—knock on wood—getting as sick now because the bacterial load is going down, and I think I have a pretty good detox routine.” On the day following a stinging session, the women typically soak in Epsom salt baths, dry brush the skin around their lymph glands, and take coffee enemas—an effort they believe will expel toxins.
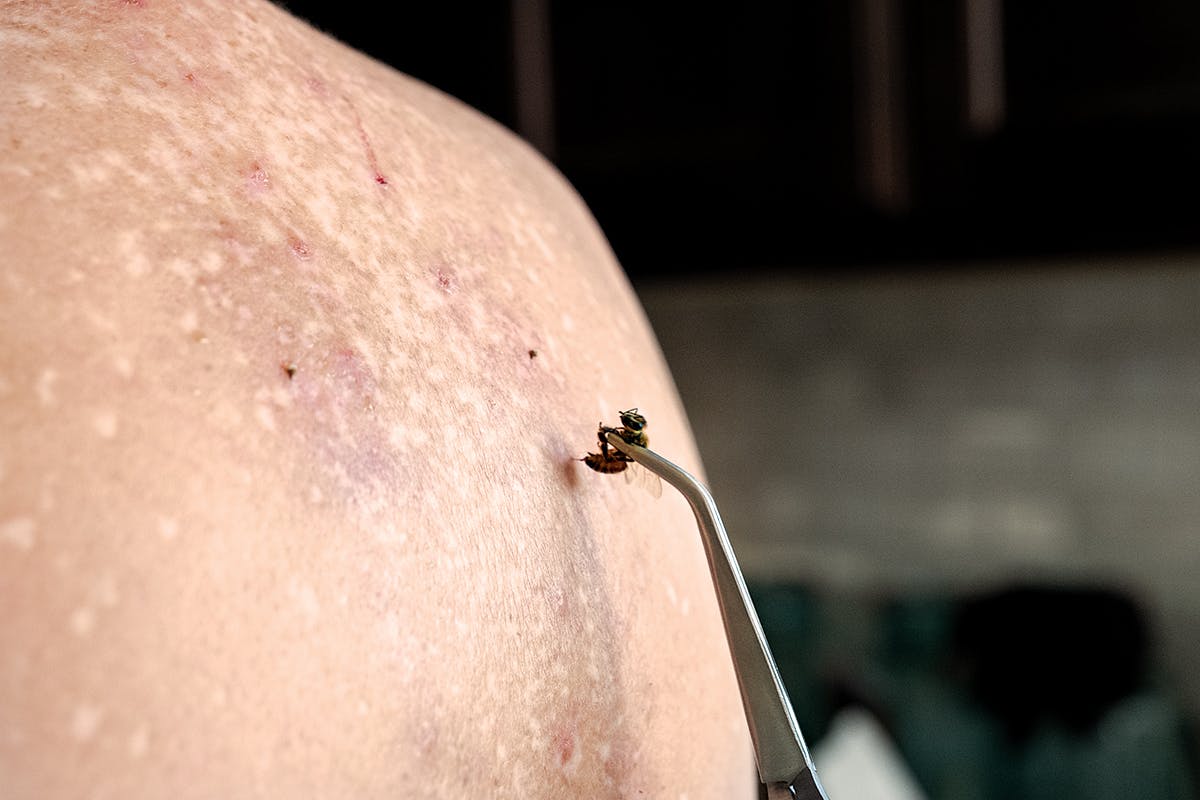
Like a nurse giving a vaccine, Gschwind held a bee in tweezers as Avery removed her ice pack. “Okay, ready?” Gschwind asked. “One, two, three.” She held the bee’s butt about an inch to the left of Avery’s lower spine and waited for the tiny stinger to pierce the skin. Then she pulled away the bee, now missing its stinger, which was still drilling into Avery’s back. The vibrating fuzzball was doomed without its barb, and Gschwind placed it in some soapy water to hasten its inevitable end. Afterward, Avery grimaced and breathed deeply as she returned the ice pack to her lower spine, preparing for the next sting.
This process would continue until the bottom portion of Avery’s spine looked like a clear highway running between two parallel rows of five inflamed bumps. Each protrusion was dotted with a stinger, moving like a pumpjack atop a tiny, rising hill, as it continued to gently, rhythmically, excrete venom. Twenty minutes later, when the barbs had done their job and stopped moving, Gschwind extracted them. Then Avery went through the same procedure to sting Gschwind.
While everything about this routine was taxing—the stinging, the seeming Herxheimer reaction, collecting bees and keeping them in her apartment—Gschwind didn’t see much of an alternative. She could not sit on the couch and groan in pain year in and year out while doctors told her she was fine, or that she should be fine, or that she would feel better in time. She’d tried that already. “What am I going to do? Because this isn’t fair. I deserve to have a life, to be functional,” she said. “Well, I guess I’m going to stick myself with bees.”

Growing up in the Chicago suburbs, Gschwind was a happy kid who spent all day at the pool or playing outside until the streetlights signaled dusk. After she graduated from college, she was a striver in a rush to become an adult; by age 23, she’d already married, landed a marketing job, and bought a three-bedroom house. She’d planned out her years, and she was enjoying an orderly life of work, book clubs, and backyard parties. “I did everything right,” she said.
Gschwind’s troubles started one day in 2009 when, sitting at her office desk, she noticed an itchy scab that seemed to have been caused by a bug bite near her right Achilles tendon. Later, she saw the spot was surrounded by a palm-sized rash. She wasn’t sure where she’d been bitten—maybe in her office’s parking lot, which was surrounded by fields, or at a barbecue at a friend’s house. Looking back, she would realize that it was after the appearance of the bite that she began to feel increasingly tired. Over time she came to feel so exhausted that she couldn’t lift her forearm to reach a glass of water in front of her, and she went to a doctor. But because she hadn’t been hiking or camping in the woods recently, the doctor assumed it wasn’t Lyme disease.
Eventually misdiagnosed as autoimmune arthritis, her symptoms worsened. Her joints ached and swelled, possibly aggravated by the changes in barometric pressure during the cold Chicago winters. By 2011, two years after the bite, she’d had to stop working full-time, and she began forgoing the parties and book club meetings that she loved to take naps and go to doctor appointments. She was too weak to stand in the shower, and her legs were so sore she would ice them down before and after work. She experienced occasional hand paralysis, forcing her to type with her pinkies. Later on she couldn’t even think clearly, enduring “brain fog” so severe she once got lost in her sister’s two-bedroom house.
Gschwind visited the Mayo Clinic, where the doctors changed her diagnosis to fibromyalgia, a sleep disorder, and Hashimoto’s disease, in which the immune system attacks the thyroid. They recommended a pain rehabilitation clinic and told her to try to relax.
But even after she and her husband moved to Austin in 2014, hoping the warmer weather might ease her joint pain, she didn’t get better. She was mystified, frustrated with the medical community she’d always trusted. A new doctor successfully regulated her thyroid, which helped her fatigue, but nothing seemed to ease her pain. For a while, she wondered whether she might have lymphoma or some congenital disease. Then, in late 2015, she saw an interview on TV with Lyme sufferer Avril Lavigne, in which the singer described symptoms identical to Gschwind’s. She began searching the internet for solutions, and decided, based on recommendations by Lyme patients online, to visit a doctor in Houston named Patricia Salvato. During her first visit, Salvato conducted an immune system blood test on Gschwind, albeit one not accepted by the Centers for Disease Control and Prevention as a good indicator of infection. Afterward she told Gschwind that she didn’t have fibromyalgia, a sleep disorder, or arthritis; she had Lyme.
Gschwind had read just enough to know that she was stepping into a minefield of modern medicine. Lyme disease is one of the fastest-growing illnesses in the United States. The CDC estimates that roughly 300,000 people receive a conventional diagnosis of Lyme each year—more than for HIV (about 39,000 per year) and breast cancer (245,000) combined. It was identified as an illness in 1975, when sufferers in Lyme, Connecticut, reported a mysterious outbreak of arthritis and juvenile arthritis. In 1982 the entomologist Wilhelm Burgdorfer discovered the source of their misery—a spiral bacterium spread by the Ixodes deer tick- that would come to be named Borrelia burgdorferi. In time, the tick broadened its reach from the East Coast to the rest of the United States, as more people came into proximity with tick hosts such as white-footed mice, which have been taking advantage of increasingly warm winters to procreate and expand their territory, and deer, prevalent in new subdivisions that used to be forest.
Medical breakthroughs sometimes begin with an outlandish- sounding idea, but without expensive, well- designed clinical trials, any proof of a treatment’s success will remain elusive.
But long after the cause was identified, the nature of Lyme—how best to diagnose it and treat the cases that linger—remains fiercely debated. The trouble begins with the tests for Lyme disease, the most-accepted of which are criticized for inaccuracy, while alternative methods of diagnosis are not widely embraced. Because of that uncertainty, some patients who believe they have the disease may not have it. Then again, they might. In one study, a Lyme researcher at Tulane University, Monica Embers, infected ten monkeys with Borrelia burgdorferi bacteria; two of them didn’t test positive for Lyme antibodies, which is currently the only means of testing for the disease. “Just because you have a negative lab test for Lyme does not mean you don’t have Lyme,” she told me.
In the best-case scenario, that of a person with an obvious “bull’s-eye” tick bite who is quickly diagnosed, a few weeks of antibiotic treatment should knock out the bacteria and the symptoms that accompany it. But even in some of those instances, symptoms persist, leading doctors to wonder if the bacteria are still present or if an autoimmune response is to blame. The symptoms can mimic everything from fibromyalgia, chronic fatigue syndrome, and multiple sclerosis to amyotrophic lateral sclerosis (ALS), Parkinson’s disease, and Alzheimer’s disease. (Lyme is sometimes called “the great imitator.”) Further complicating matters, the Ixodes tick can also transmit anaplasma, babesia, Borrelia miyamotoi, the Powassan virus, and other pathogens that can lead to organ failure, neurological degeneration, and death. Lyme patients sometimes see improvements when they take antibiotics for longer periods, though critics attribute that to a placebo effect and warn against long-term antibiotic use.
The Lyme diagnosis left Gschwind with mixed feelings. She was relieved to have what seemed to be an answer, yet when it came to Lyme, she wasn’t sure what to think, and her internet research didn’t help (as usual), providing conflicting information and horror stories at every turn. After her visit to Salvato, she took oral antibiotics for four months. She felt a little less pain and a little more energy, and then her health plateaued. She traveled to California to consult with a doctor there, and he prescribed herbal remedies that cost $2,000 to $5,000 a month. She racked up about $20,000 in debt over a year and a half. Her expenses were soaring beyond anything she could repay. Worse, her husband, burned out from constantly worrying and taking care of her, asked for a divorce in 2017. She was now alone and running out of options.
One day, Gschwind was in the shower when she became overwhelmed by despair. “I thought, ‘There’s no way I’m going to make this. There’s no way I’m going to live,’ ” she said. “I had this sudden, extreme sense of impending doom and extreme sadness hit me out of nowhere and so I got out of the shower and put on a towel and called the suicide line.” Another time Gschwind had suicidal thoughts, she said, she texted the hot-line, crying so hard she couldn’t talk, and began giving the counselor a carefully thought-out argument about why her dying would be best for everybody.
By the spring of 2018, Gschwind was broke and growing dependent on her mother to pay her bills. Searching for alternatives to the expensive herbs for Lyme, she saw positive internet testimonials about intravenous antibiotics. “I really wanted to do the IV antibiotics, but I was just like, ‘There’s no way I can pay for this.’ They cost $10,000 to $20,000 a month,” she said.
Bee venom was a last resort. She’d heard about it in Austin at an informal Lyme disease support group—a handful of women who’d found each other through Facebook. Miriam Shannon, a no-nonsense, 58-year-old nurse with a military background, had been taking antibiotics and, after a long stretch of unemployment, was feeling well enough to resume full-time work, as a nurse in a downtown jail. But at a Lyme awareness march in Washington, D.C., she had learned about the bee venom protocol, and she and another Austin-based Lyme sufferer began stinging each other. When her friend announced she was moving to Denver, Shannon told Gschwind she needed a new stinging partner.Gschwind had always hated bugs and was scared the first time she lifted her shirt to expose her back at Shannon’s house. “I knew it might not work, or my body might hurt. But I knew this is what I have to do or I have no chance of living,” she said. She noticed a difference afterward—she was more flexible—though it took a few months to see significant overall improvements. Her joint pain flared up less frequently. She could form complete thoughts again, making it easier for her to return texts and phone calls. Her energy came back once in a while, and she could get off the couch more often without overtaxing herself. Gradually, she felt her old self returning. She began thinking about part-time work.
The duo would become a trio as Gschwind and Shannon recruited Avery, a former paralegal they knew from the support group. In time, they settled into certain roles. Shannon was the mother hen, because of her age and experience; she was the group’s living proof that stinging worked. Gschwind was considered “the brain,” because when she was thinking clearly, she was eager to synthesize and share new information. Avery was the newbie, living with her mom, still too sick to get a full-time job. In addition to stinging together, the friends relied on one another for emotional support, talking about their pain, their medical bills, their divorces, and the frustrating relatives and friends who thought they were faking symptoms to get attention. They believed one another, and they believed other Lyme sufferers. They came up with a name for their group: the Hive Tribe.
Apitherapy—enlisting bees and bee products for medicinal purposes—has been practiced around the world for thousands of years. Ancient medical texts would recommend bee-related cures for everything from toothaches to female sterility. The English beekeeper Tickner Edwardes wrote in his 1907 book The Bee-Master of Warrilow about the experiences of a fellow beekeeper who was also a physician. The doctor approached a man with “rheumatism” and administered a half-dozen stings, and the man “passed from whimpering through the various stages of growing indignation to sheer undisguised profanity.” Noting that the patient would get better, the doctor told Edwardes, “There is nothing new in this treatment of rheumatism by bee stings. It is literally as old as the hills. Every bee-keeper for the last two thousand years has known of it.” Many beekeepers continue to claim that they don’t get arthritis.
Whether it works for Lyme disease is another question entirely. Researchers often approach medicinal bee venom as skeptically as they would magic crystals or lucky charms. But some aren’t ruling it out. “In principle, it is conceivable that you do something unusual, like a bee sting, and that’s going to help a disease whose nature we do not understand,” said Kim Lewis, a Lyme researcher and director of Northeastern University’s Antimicrobial Discovery Center, in Boston. “But without a proper clinical trial, it’s hard to tell whether this is for real.” Noting that patients are desperate, Monica Embers of Tulane stressed the importance of well-designed studies. “We want to find something that works,” she said.
The woman who claims to have invented the ten-sting protocol for Lyme disease is Ellie Lobel, a 51-year old Californian with a complicated backstory. She claims that she got a PhD in nuclear physics from the University College Kensington, in England, at age eighteen, and that she later worked on a secret project for the U.S. government, which she couldn’t discuss—a résumé often repeated without question in publications profiling her. When I told her I was having difficulty finding any evidence of a “University College Kensington,” she said that it was “dissolved long ago,” and explained that any documentation of her life before her involvement with Lyme therapies is classified. She only mentions her résumé, she told me, to let people know that she “was a little smarter than the average bear” and that she “knew how to research and problem-solve and put things together.”
The tale Lobel tells reporters has become a sort of origin story for those who use bee stings to treat Lyme. In 2011, she says, she had been sick with Lyme disease for fifteen years, and her condition had deteriorated. She had been confined to a wheelchair, she claims, and was experiencing multiple organ failure. Though she’d tried unconventional and conventional treatments, including antibiotics, a doctor gave her just a few months to live. Then one day, on a rare venture outside with a caretaker, she was stung by a swarm of bees. The caretaker ran, Lobel says, though she could not. While the stings were painful and terrifying, she figured that they would bring on a swift death. Swollen and sicker than she’d ever been, she went into septic shock for three and a half days, waiting in bed to die. In the aftermath, to her surprise, the pain lifted. The relief only lasted a few hours, but the experience gave her an idea, she said, that bee venom could help her.
When I asked Lobel if I could talk to the caretaker, she gave me the name of John Husted, warning me that they were estranged and hadn’t spoken in years. I called Husted, a 58-year-old surgeon in California, and asked him about Lobel’s bee attack.
He seemed to be summoning up a distant memory, speaking slowly. “She had chronic Lyme and she got stung by a bee, actually—which is never fun, being stung by a bee—and then she felt better afterwards,” he said. Assuming he would’ve recalled a swarm of bees that nearly killed a woman in his care, however long ago, I waited for him to elaborate. Husted continued, “It got started when she was stung by a bee—stung by two bees, I think it was—and she noticed that she kind of felt better. I know that was something that got her interested in apitherapy as a patient, and then she became a big voice within bee venom.” He hung up soon after and has not answered repeated requests for further clarification.
Lobel, meanwhile, stuck to her story. “Sometimes truth is stranger than fiction,” she wrote me in an email. While Lobel was stinging herself, creating the protocol, she also developed an anti-aging bee venom face cream called BeeVinity. A California manufacturer named Steven Riscol told me that when he worked with Lobel to create BeeVinity, in 2012, he heard about the swarm attack from both Lobel and Husted, though by that time “she was very healthy.”
Bee venom therapy soon became Lobel’s mission. She began emailing instructions to Lyme sufferers and visiting Facebook friends in person, sharing her approach. In 2015, after copyrighting the protocol, she set up a Facebook group called “Bee Venom Therapy For Lyme Disease.”
“I have to remind myself why we’re stinging,” Gschwind said. “I’ll question: ‘What the heck am I doing? This is weird. This is stupid. Why are we doing this?’”
Many who tried the procedure reported that it was working. One of the first people to follow her instructions was a Facebook contact named Nancy Dolan, a restorer of historical buildings in St. Louis who had had Lyme disease since 1998. When Dolan first heard about bee venom therapy, she said, she was fifty years old and bedridden with symptoms of Parkinson’s disease and ALS. “By the end of the first year of stinging, in 2014, I had my life back,” she told me. Eight months into stinging, she said, her doctor took one look at her and burst into tears: “She asked to take a picture. She didn’t try to explain it.” Dolan is now working full-time as a hypnotherapist and firmly believes in the placebo effect, though she’s unconvinced that it alone would account for the dramatic change in her health. She told me that her medical bills over her entire Lyme journey mounted to around $1.5 million and that all the treatments she’d had in the past were unable to achieve bee venom’s striking results.
In the years that followed, an increasing number of Lyme sufferers started using Lobel’s technique, with good outcomes. Not only did they say they felt better, they said that it saved their lives. Wanting to combine Lobel’s protocol with a more holistic approach, Dolan started a Facebook group of her own called “Healing Lyme With Bee Venom,” where more than 5,500 members post their questions and testimonials. “Year 1 was rough on my husband,” wrote the spouse of one Lyme sufferer who used the bee therapy. “Yesterday he walked seven miles hiking thru a state park.” “I was bedridden when I first started and I more or less lead a normal life now,” said another group member.
It is possible—some would say probable—that these individuals are promoting a technique whose success is based more on psychology than pharmacology. There is little science to substantiate a cure by stinging. There have been two clinical studies investigating the link between bee venom and Lyme, and though they are compelling, they are confined to petri dishes. A 1997 study and a 2017 study showed the interaction of bee venom’s primary component, melittin, and the Lyme bacteria, Borrelia burgdorferi. Melittin, which is a helical peptide consisting of 26 amino acids, tends to bore a hole in the outer membrane of the larger, spiral-shaped Borrelia burgdorferi, releasing the inner contents of the bacteria just as a corkscrew would slice open a water balloon.
Yet these in vitro experiments don’t translate to the human body. For starters, bees don’t carry enough venom to have more than a local effect. This is a good thing, experts argue, because if the venom did reach the bloodstream in a dose large enough to be effective against the bacteria, it could kill the patient. “Many things are antibiotic—like bleach,” said Sam Robinson, a venom researcher at the University of Queensland, in Brisbane, Australia. “Bleach is effective at killing any microbe, but you can’t use it as a drug.”
Perhaps, instead of destroying the bacteria directly, the venom’s effect is indirect, kick-starting the immune system. Bee venom studies have shown promise in combating symptoms for autoimmune diseases such as multiple sclerosis and rheumatoid arthritis. According to Justin Schmidt, an insect venom expert at the Southwestern Biological Institute, in Tucson, it’s possible that when the immune system begins attacking itself, an injection of bee venom may help by providing an alternate target—“something to chew on,” he said, “and this tends to regulate the immune system so it does what it’s supposed to be doing, which is attack toxins that are getting into your body.” While Lyme is a bacterial infection, it sometimes mimics autoimmune disorders, and so maybe, somehow, similar rules apply.
It’s also possible that the pain of the stings plays a role. “Maybe the venom is doing something to kick off pain receptors,” he said. Anecdotal evidence suggests that other types of venom may also work this way. A brief article in the Lancet, from 1983, described a 43-year-old woman in Arizona who had MS and went into remission for two months following a scorpion sting on her right foot. An immunologist in Houston told me she was contacted by a physician experiencing progressive MS who said he’d been stung by a sea anemone and went into temporary remission.
Medical breakthroughs sometimes begin with an outlandish-sounding idea, but without expensive, well-designed clinical trials, any proof of a treatment’s success will remain elusive, any rationale speculative. “These are wonderful questions, hard to answer,” Schmidt said. “The problem is that you can’t make any money off bee venom because you can’t patent it, so nobody is willing to do the research to see if it works.” Outside the pharmaceutical industry, the government could fund a study if researchers found some promise in bee venom, though right now that scenario is unlikely. Bee venom has been stigmatized as folk medicine, quack science, and that’s a difficult reputation to shake.

In the absence of clinical trials, bee venom users rely on the power of anecdotes. One day, I went onto Dolan’s bee venom Facebook page and posed a question: How many people in the group had gone into complete remission after following the bee-sting protocol for two to three years? Ten people responded that they were healed, and a woman who had been keeping count on the site commented that the number hovered around sixty. “Fully recovered, did bvt [bee venom treatment] 4/15-8/17. Was disabled etc. Fully functional now. Working full time, running etc,” responded one woman. Another wrote, “I went from non-functioning, wheelchair-bound human to a functioning, happy, grateful survivor.”
Given their devotion to venom therapy, it was no surprise to find the Hive Tribe spreading the gospel at Buzzfest, a bee-product festival held this spring at the BeeWeaver Honey Farm in the East Texas town of Navasota. Vendors sold flavored honey, CBD-infused honey, and mead; they handed out recipes for things like honey hummus and honey-balsamic beef; they sold T-shirts bearing bee puns and phrases like “Game of Drones” and “Comb Sweet Comb.” Two young women walked the grounds in tiaras and sashes proclaiming them the “2019 American Honey Queen” and “2019 American Honey Princess.” Someone brought her pet pig, Juliet, dressed in a yellow-and-black tutu.
Huddling under a bright yellow canopy for shade, two beekeepers named Sandi Murray and Cyrus Nasr, of the Hive Bee Farm in Houston, were giving about a dozen spectators a presentation on the honeybee’s healing benefits. Nasr stressed to the crowd that he and Murray were not doctors and they were not dispensing medical advice; they were merely relaying their observations. Yet their claims had a throwback quality. Propolis, a substance bees make to seal their hives, boosted the immune system, they said. Air sucked out of a hive alleviated emphysema and chronic bronchitis. It corrected sinus infections. Stinging reduced inflammation in joints. One woman the couple treated had crippling arthritis, they said, and by the third stinging session, “she threw away the cane!”
When they spotted Avery, whom they’d met previously and invited to the demonstration, they motioned to the Hive Tribe. “So why don’t you guys talk a little bit about Lyme disease?” Nasr asked. Not one to disguise her enthusiasm, Avery was wearing hexagonal, honeycomb-shaped earrings and a “Bees Please” T-shirt. She introduced herself and her friends as Lyme disease survivors who’d become desperate for relief and were healing themselves with bee venom therapy.
“Doctors don’t believe that you have it,” Avery said, at one point. “They’ll tell you, ‘You do not live in the Northeastern states, so you don’t have Lyme disease; it doesn’t exist in Texas.’” (The Texas Department of Health and Human Services typically records an average of around ninety cases of Lyme annually.)
An agitated woman sitting in a folding chair in the middle of the tent seemed to have been waiting for this moment and said, “I even gave them a tick and the tick came back with it, and they still told me no! That’s crazy!”
Presenters interviewed the Hive Tribe throughout the day, and Murray demonstrated how to sting someone for therapeutic purposes. Once, she used tweezers to hold a bee near Nasr’s forearm, awkwardly negotiating around his thick arm hair. As she tried again and again, the audience remained captivated, angling for a good view. One older woman, stifling a giggle, asked: “Is there a way to get the bee venom without having to get the sting?”
A man in the audience named Victor Herrera leaned back on his heels and piped up: “Well, you can get injectable venom.” He was a beekeeper, he said, and his wife, who was seated in a chair next to him, had Lyme disease. They, too, had been using Lobel’s protocol, though he’d noticed that in the winter, his wife wasn’t improving as quickly as she had been in the summer. Theorizing that winter venom wasn’t as strong, he turned to European drugmakers who’d been selling venom. “We think it is the best thing; that’s our personal opinion,” he said. “I’m not saying it wasn’t working with the bees. It was working. It was just up and down, up and down.”
Gschwind and her friends were intrigued by this couple and eagerly approached them. “I’ve noticed in winter the bee sting seems weaker,” Shannon said. “But when summer comes around, man.”
“Yeah, yeah, yeah,” Herrera said. “Summer bees are fantastic.”
As the Hive Bee Farm couple continued their talk, Gschwind and the other bee-sting missionaries discreetly moved their conversation outside the tent. Herrera explained that the injectable venom provided the equivalent of about forty bee stings per bottle and cost one hundred dollars. The women looked at one another as they did the math.
They had never considered that melittin concentration might vary. Discussing the matter on the way home, they decided that the benefits wouldn’t justify the price. While injectable venom was cheaper than most treatments, it was still more expensive than bees, and none of the women was in great financial shape. Avery threw away her old medical bills, absolving herself with the justification that she didn’t have any money. Gschwind owed tens of thousands of dollars in credit card debt. Shannon was finally in the black, having filed for personal bankruptcy in 2010, when she owed nearly $100,000 in medical bills.
Though Herrera had piqued their curiosity, they’d already made a different plan.


The day after Buzzfest, Gschwind and Avery left their houses for a second day in a row. Usually, they would be too tired to do such a thing; they would stay in and sleep. That Sunday, however, they had an incentive. They were going to buy a hive.
Shannon had owned a hive, until it collapsed this past winter, leaving the trio to rely on other local beekeepers, like the one who’d met Gschwind at Whataburger. “I don’t know exactly what happened,” Shannon told me. She’d put a damp rug on top of the hive during a cold snap and brought it into her garage. When she checked on the bees the next day, they were dead. “I grieved for a long time,” she said. “I was so pissed.”
By springtime, she had found a hive for sale at a bee farm outside of San Antonio called the Bee Place, for $250, a fee she planned to split three ways, and since she was working most days the hive was available for pickup, Gschwind would have to go instead and bring the hive back in the trunk of her car.
Gschwind barreled down I-35 toward San Antonio, while Avery kept her company. The friends talked about past relationships. They talked about the ways in which Lyme has put their priorities in perspective. Avery went quiet for a while, watching the strip malls and box stores go by. Then she mentioned how, when the illness was at its peak, she’d imagined ending her life. Gschwind acknowledged she’d had the same impulse. “I would be driving, and then all of a sudden, I’d have an unwanted thought of me flying off the road,” Gschwind said.
She assured Avery that, sitting in the car at that moment, she didn’t want to die—it had been the disease affecting her thoughts. But she admitted to worrying a lot. “Even if I do survive this, the damage that it has done to my body—I mean, I’m not married; what is going to happen to me?” she said. She could only hope that something would turn her life around, a hope that seemed to pass like a ladder among the two of them and Shannon, so that one, at least, could hold out a hand to help the others up.
A few miles southwest of San Antonio, in a bucolic clearing just off a quiet, rural highway, a beekeeper named Gary Rankin was doing his best to calm a disrupted hive. Preparing for transport was bound to set off the bees. They were flying out of the hive and circling, and since he wasn’t wearing the vented helmet of his beekeeper suit, his face offered them a fleshy pink target.

Seeming no more bothered than a man enveloped by butterflies, he smiled widely and approached Gschwind’s car wearing sunglasses and a white sweatband to hold back his spikes of white hair. Though Gschwind stings herself with bees thirty times a week, she prefers to control when she gets stung, and she kept her window open just a crack while conducting business. She and Avery were using the bees as a Lyme disease treatment, she told Rankin, bracing herself for the typical baffled reaction.
“Lyme?” he said, unsurprised. “I’ve heard people were buying bees from me for that reason. You know, it’s a roller-coaster ride that everybody seems to get off happy at the end.” He guessed he’d had about a dozen customers in the past few years buying bees for Lyme. Gschwind told him they’d tried other remedies, without success. Rankin nodded as he listened, recognizing that their experience was common. “That’s the story I’m hearing. You go through all the Western medicine garbage, and that doesn’t work, and now you’re here,” he said.
The Hive Tribe liked the idea of pioneering a new cure that could be vindicated at some point in the future. Maybe they’d even be seen as heroes instead of nutcases. Maybe someday, someone would ask them about the early days of bee venom therapy and want to hear their stories.
On the return trip to Austin, Gschwind and Avery seemed more tired than usual. They admitted they’d been worn out from the day before, though they’d tried to hide it from me. Once I’d left, they said, they’d become whiny because they had to sting. “We were like little babies,” Avery said. “She’s like, ‘I’m so tired; I can’t believe we’re stinging. This shit sucks.’ ”
“I have to remind myself why we’re stinging,” Gschwind said. “Like I have to seriously look for it when I’m in that much pain. I’ll question: ‘What the heck am I doing? This is weird. This is stupid. Why are we doing this?’ ”
Then Avery would remind her, “We’re trying to get better.”
This article originally appeared in the December 2019 issue of Texas Monthly with the headline “The Sting Operation.” Subscribe today









