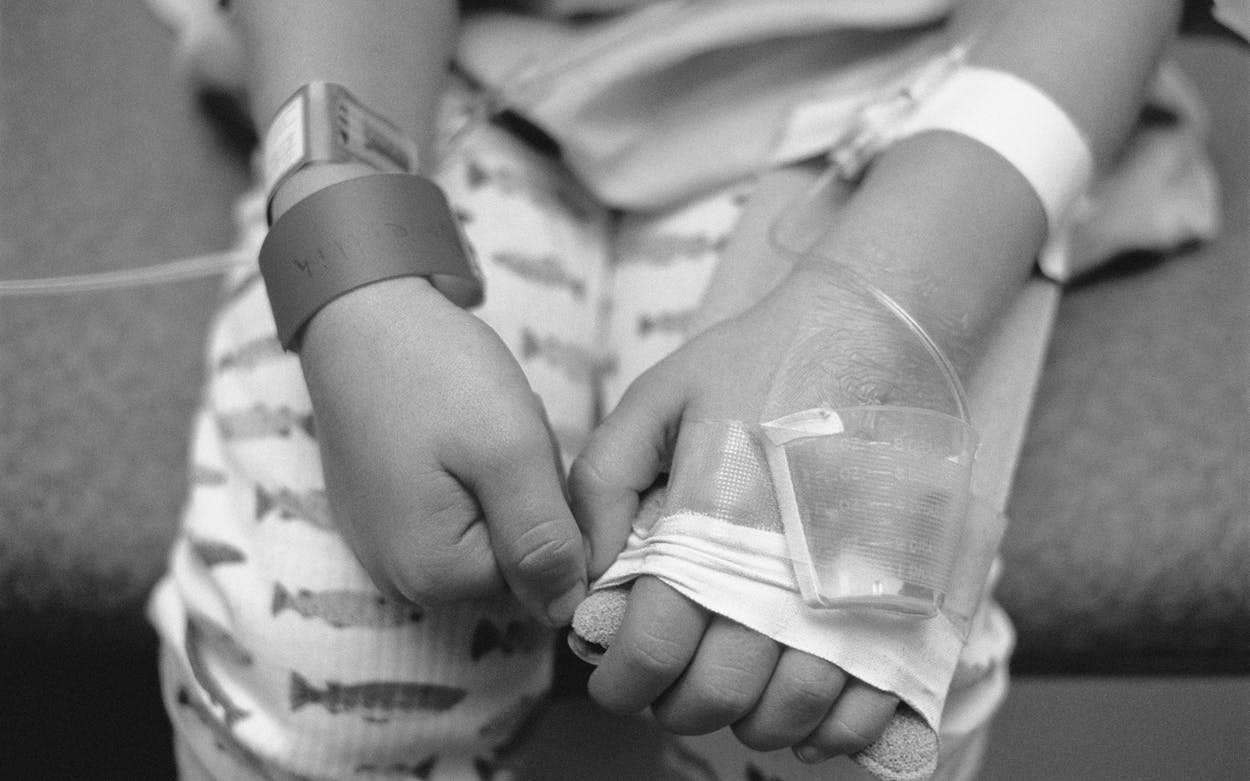
It wasn’t unusual for Harper to fall suddenly. “She’s a toe walker,” said her mother, Brooke Wilson, referring to a condition associated with her daughter’s autism. “She’ll literally just be standing there, and she’ll tip over.” But this time was different.
One morning last fall, Wilson was getting ready to go to her job as a special education teacher when her husband called out from the kitchen. She rushed in to find nine-year-old Harper slumped over, with her head on the counter. When Wilson lifted Harper’s face, the girl’s eyes rolled back, and her body crumpled downward. “Thank God I was right there, so her head didn’t hit the floor,” Wilson said. “It was the scariest thing. My whole body was shaking.”
As the family rushed to an emergency room in Fort Worth, about fifteen miles north of home, in Burleson, an extra stressor creeped into Wilson’s mind: the cost of the hospital visit. “We didn’t know how much it was going to be. We didn’t know what was wrong with her. We didn’t know if we were going to have an extended stay,” she said. “But mainly, we just wanted her to get better.”

Just weeks earlier, Harper had been kicked off Medicaid, the state-administered health insurance program she had relied on for most of her life. She and her twin brother, whom Wilson calls “miracles,” were born more than three months premature. Harper spent more time in the neonatal intensive care unit—eight months—than in utero. She came home with a tracheal tube to help her breathe and a gastrostomy button through which she could be fed. She still requires care for chronic lung disease and serious digestive issues.
While Wilson and her husband have private health insurance, they depend on Medicaid for the specialty care necessitated by Harper’s disabilities. This has included occupational, physical, and speech therapies, as well an in-home attendant who helps Harper eat, perform daily tasks, and learn to live as independently as possible. So a letter from the Texas Health and Human Services Commission that arrived in mid-September brought the couple shock and distress in announcing that Harper’s benefits would end October 1 because they had failed to provide the agency certain tax information.
Harper is among 1.8 million Texans who have been removed from the health insurance program since April 2023, and one of more than 15 million nationwide, following the end of a three-year federal moratorium on disenrolling anyone during the COVID-19 pandemic. The pause offered respite for families from what advocates have long said are overly burdensome checks that previously led to thousands of eligible Texas kids losing coverage each month. Wilson had known that the state would resume checking the eligibility of millions of Medicaid recipients last spring. But she thought Harper wouldn’t be affected because she had Medicaid through a waiver program due to her long-term disability, and therefore shouldn’t have been subject to regular checks, according to her attorney at Disability Rights Texas, a legal advocacy group.
Texas, which for years has had the highest rate of residents without health insurance of any state, by a wide margin, also has the highest Medicaid disenrollment rate in the country since the moratorium was lifted, according to the Kaiser Family Foundation. More Texans have been kicked off Medicaid in the last nine months than live in San Antonio, the state’s second-most populous city. The majority are children.
At the hospital after Harper’s fall, doctors treated her for strep throat and dehydration, giving her IV fluids and antibiotics. Without Medicaid, Harper had been forgoing her physical therapy appointments, which cost $150 each week, and Wilson couldn’t help but wonder if that contributed to the ER visit. “The more she moves, the better her digestion is,” she said. If Harper had been doing her regular exercises, she might not have collapsed. “Maybe [she] would have. But she’s never done that before.” The family was able to return home that evening, but in the weeks that followed, bills piled up, and the couple had to start paying Harper’s home health aide about $1,000 each month out of pocket.
Adding to the frustration of Texans who have lost Medicaid in recent months is that most of them, including Harper, weren’t actually deemed ineligible for the program. Nearly 1.2 million were removed for “procedural” reasons, stymied by the red tape of the renewal process. As of last month, this included more than 858,000 kids. In some of these cases, according to Medicaid advocates, families moved and never received the letter informing them that they needed to submit certain income information, or the notification was written in a language they don’t read, or they submitted paperwork but it was missing a signature, or they needed assistance renewing their coverage but couldn’t get through to HHSC by calling 211.
Terry Anstee, an attorney with Disability Rights Texas, said he’s seen situations in which the state determined people no longer qualified for Medicaid under one eligibility criterion and removed them, even though they were eligible under another. Other applicants appeared to have done everything right but were erroneously kicked off anyway. In a couple of confusing cases, Anstee said, people who qualified due to a disability were kicked off Medicaid and moved to the Healthy Texas Women program, which offers a completely different set of services. “It was just nonsensical,” he said. “I don’t know if it was some sort of computer glitch—I really don’t know.” Asked about such apparent technical errors, Tiffany Young, an HHS spokesperson, said the agency had identified 100,000 Texans who were “denied improperly” and “worked quickly to reinstate coverage.” The agency, Young wrote in an email to Texas Monthly, was “taking all possible actions to provide benefits to eligible Texans as quickly as possible.”
While other states have relied more heavily on first checking eligibility through readily available data sources, Texas has renewed fewer than 3 percent of Medicaid enrollees this way—the lowest rate in the country. Instead, the state health commission has generally required the submission of renewal paperwork that patient advocates say has further bogged down an eligibility system that was already understaffed, overworked, ill-equipped, and chronically underfunded, even before it tried to process a monumental number of renewals in a span of months. Backlogs of both Medicaid and SNAP food assistance renewal applications ballooned, leading to wait times as long as several months.
Meanwhile, Young said the agency has responded to the increased workload by trying to recruit and train new eligibility staff members and moving workers from other areas to help process renewals. It has also relied on overtime work from staff, because “it takes a new eligibility adviser a year to be proficient with application processing, and overtime is the most readily available tool to address workload quickly,” she said. In one instance, the agency offered raffle prizes for workers who completed at least fifteen hours of overtime in the first week in December. As of the end of last month, 305,390 Medicaid renewal applications were pending, Young said, with a wait time of 39 days.
According to advocates and providers, some patients are showing up for appointments only to learn that they no longer have Medicaid and can’t afford to pay out of pocket to be seen. Even if their coverage is eventually restored, gaps can mean children missing vaccines or patients forgoing treatments for chronic diseases. Shanna Combs, president-elect of the Texas Association of Obstetricians and Gynecologists, said she’s heard about pregnant patients losing Medicaid just weeks before their due dates. At her practice in Fort Worth, she saw a child who was admitted to the hospital with a blockage in her lower genital tract, only learning then that she was no longer enrolled. “She basically has a uterus full of blood that’s probably up to her belly button” and needed MRI imaging and ultimately surgery that the family couldn’t afford, said Combs. Doctors had to wait several weeks for her Medicaid to be reinstated, giving the child medication to try to prevent the condition from worsening in the meantime.
There are also broader effects from this lost coverage on safety net clinics and hospitals, which have long been buckling under the weight of the state’s uninsured population, as the governor and the Legislature continue to refuse to accept federal funds that would expand Medicaid access. “It feels like you’re in a boat that’s sinking, and you’ve got a little bitty Dixie cup, and you’re trying to get the water out of the boat before you sink,” said Jana Eubank, executive director of the Texas Association of Community Health Centers, a nonprofit representing federally funded clinics that last year served close to two million Texans regardless of their ability to pay. Eubank said these health centers greatly depend on payments from Medicaid to help offset the cost of treating uninsured patients. “We’re going to have some centers that this is going to totally destabilize financially,” she said of the Medicaid disenrollment. “It keeps me up at night.”
Stacey Pogue, a policy analyst at the left-leaning advocacy nonprofit Every Texan, characterizes the recent disenrollments as indicative of a state Medicaid system that has long seemed designed to exclude, rather than include, as many patients as possible. “What this paperwork does, what the barrier does, is kick eligible people off because they missed the deadline, not uncover waves of lottery winners that are ineligible that should be removed,” she said. “That’s the trade-off, as a state where, to us, program integrity means making sure not one ineligible person is on, even if that harms a thousand eligible people.”
In late December, Disability Rights Texas sent a letter to the state health commission on Harper’s behalf. Later that same week, Wilson said she heard from the agency that Harper’s Medicaid had been reinstated. She hopes the family will be reimbursed for the services Harper received after her coverage lapsed, but she says there’s no guarantee. Harper’s walking and balance are now three months behind where they might have been because she missed out on physical therapy, and she lost her spot at the facility while she was without coverage. The family is still waiting to hear if she can resume treatments there.
Wilson told me she wishes that more parents knew they could fight these denials—maybe then the state wouldn’t make it so difficult to stay enrolled. “I hate to say this, but I wholeheartedly believe it: I feel that Medicaid just says no so parents will quit, and they almost capitalize on parents being tired and worn down by this whole process,” she said. Maybe if more people were able to fight back, officials would realize they’re wasting manpower by throwing eligible Texans off Medicaid, she thinks. Maybe they’d decide that’s not a price worth paying.
- More About:
- Politics & Policy
- Health
- Medicaid