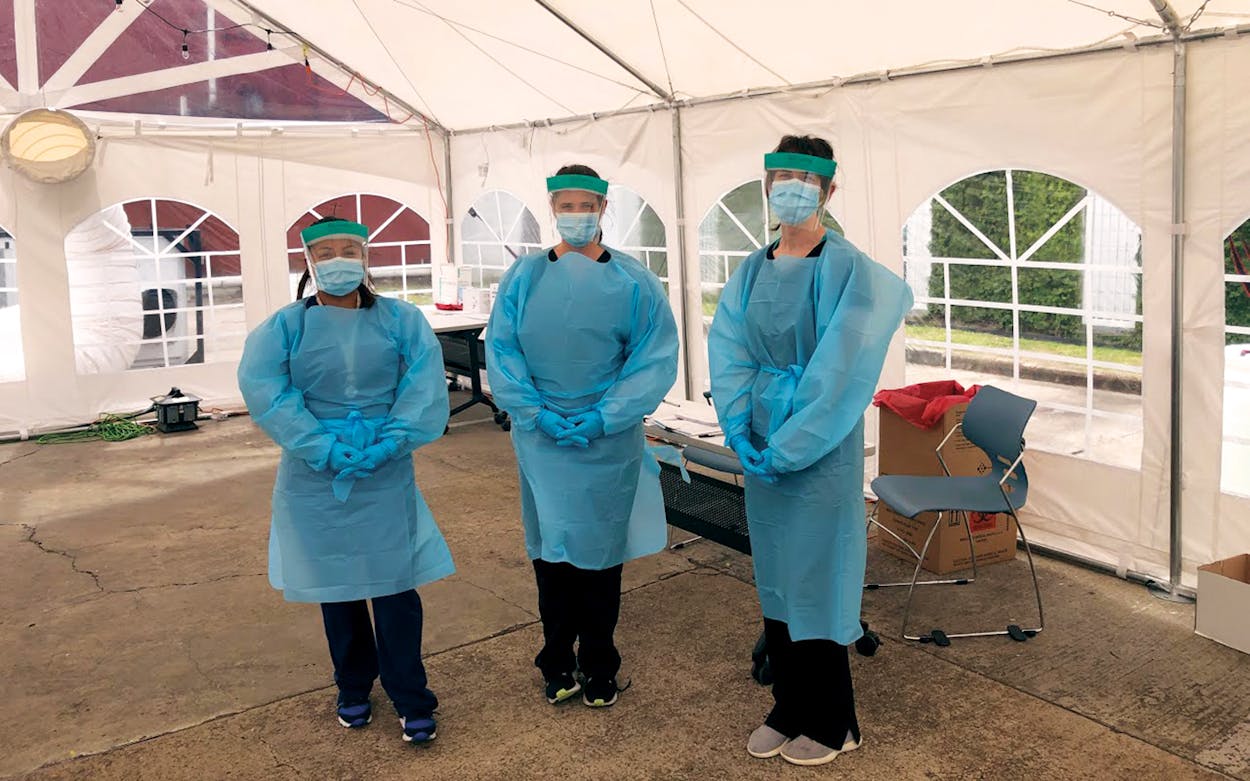
As the medical community braces for a surge of COVID-19 cases, concerns are rapidly growing over the system’s ability to handle the pandemic. This week, Katy Caldwell, CEO of Legacy Community Health in Houston, opened four walk-up tents in the Bayou City for coronavirus testing. Outside each tent, the visitors are screened and interviewed about their symptoms. Those who pass the screening then go inside the tent where a team in protective gear takes the necessary samples. Four or five days later, Legacy calls the patient with the test result.
As important as the walk-up sites are to confronting the novel coronavirus, Caldwell is also grappling with a complex set of problems. We talked to her about the challenges of keeping sick people away from healthy ones, the shortage of medical supplies, and financial threats to her business.
Texas Monthly: I’ll leave the floor open to you. What are you seeing?
Katy Caldwell: At four of our community hub sites, we now have tents set up. We’re screening people who are coming to the clinic at the door. If they meet the testing criteria, we then send them over to our tent for testing. And that’s what keeps them out of the main clinic area. And they get tested. We then contact them about the test results. You have to get out of your car and walk up to the tent.
TM: Do you think Houston will get drive-through test tents at some point?
KC: We won’t be doing it. We just don’t logistically have the place to do drive-through. The city is just now getting their drive-through sites up. In the meantime, we’re doing just walk-up testing basically. But the main thing is that we’re using the same screening criteria that the city is, that CDC is recommending that everybody use. So we’re not testing the “worried well” or people who don’t show the appropriate symptoms or don’t fall into any of the criteria that the CDC is recommending to test, which, of course, is making some people not happy.
TM: Right. What do you tell them?
KC: If they believe they’ve been exposed but they don’t have symptoms, we tell them to go self-quarantine for the next fourteen days. If they get symptoms and they really want to get tested, then they can come back. But again, you have to remember, there is right now no medication except over-the-counter medications to help people. Some of the people who come through the screen are really what we call the “worried well.” You know, they’re concerned they might have been exposed. They don’t know whether they were, but they don’t have any symptoms yet. And I think that my biggest concern so far is that we’re going to run out of masks and gloves and other personal protection equipment (PPE)—gowns, etc.—for our staff. And if that happens, it means we’re gonna have to shut down our testing for sure. And we’re going to have to be very judicious in what we do in our clinics.
TM: Because you’re having to conserve. It sounds like everybody’s having to just hang on to their one mask.
KC: Yep. Everybody’s hanging on to them. And also, you know, where we are, we’re continually—everybody, like us—is continually ordering and the suppliers are rationing everybody, especially masks and gloves. But there’s still a concern that we’re not going to have enough. One of the most important things to us right now is making sure that the people that are working at our facilities can remain safe and don’t get infected. We do everything we can so that they don’t get infected from this.
TM: It does sound like a lot of doctors and nurses are really worried about taking the virus home, especially if they have somebody who’s got a weak immune system at home.
KC: Right.
TM: What are you anticipating over the next week?
KC: I wish I could predict. We just don’t know. We truly don’t. We’ve tested about five hundred people so far. The labs are taking about four days to turn around results. So I’m not even sure we’ve gotten the results back from the first set of tests that the first day of testing that went in.
TM: Because you opened four days ago, is that right?
KC: We opened on Monday. We open two sites on Monday and then another site on Tuesday and another site on Wednesday.
TM: Is the unknown the most unnerving part of this?
KC: Well …
TM: I imagine there are a lot of things, but can you take me to that?
KC: Yeah, sure. I mean, we’re seen our regular clinic visits drop precipitously. We usually see about 2,300 people across our clinics a day and we’re now seeing about 1,500 to 1,600 a day. We get paid on a fee-for-service basis. So I’m watching the money and then knowing how many people are being laid off, furloughed, et cetera, there’s gonna be—I have a fear of that. All these people are going to lose their insurance over the next few months and then we’re going to have a big influx of uninsured adults to deal with. So, you know, it’s been watching the funding. And the other part that that’s the most unnerving is the PPE, the supplies.
TM: Any other concerns that you have?
KC: Well, number one, we’re not testing every single person because not every single person requires it. You know, I haven’t been exposed. I have no symptoms. I know I could sit here and be the worried well. I can do that to myself. But there’s only so many testing supplies. There’s only so many things that can get processed. And we want to use our supplies for the people who really, truly need to know whether or not they’ve been infected. I mean, it’s really as much a supply chain industry as anything.
TM: So it’s more like if you work in a nursing home and you suddenly feel sick, you’re gonna need to know if you just infected a bunch of people.
KC: Yes, exactly.